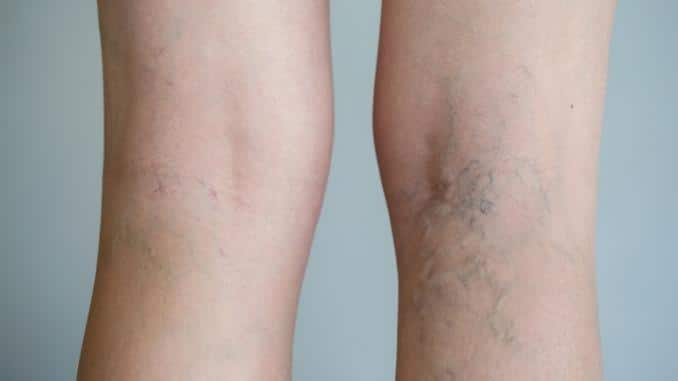
It is estimated that about 20 percent of all adults—about one-fifth—will get varicose veins at some point in their lives but there are varicose veins treatments and prevention. They are more common in older people, but younger people can get them too.
In most cases, varicose veins (also called spider veins) are simply unattractive and embarrassing. Some people, however, may experience pain and discomfort because of them, while others may be at risk for more serious complications so you can try varicose veins treatments and prevention.
If you have varicose veins, it’s important to talk to your doctor to be sure that they won’t lead to more problems down the road.

What are Varicose Veins?
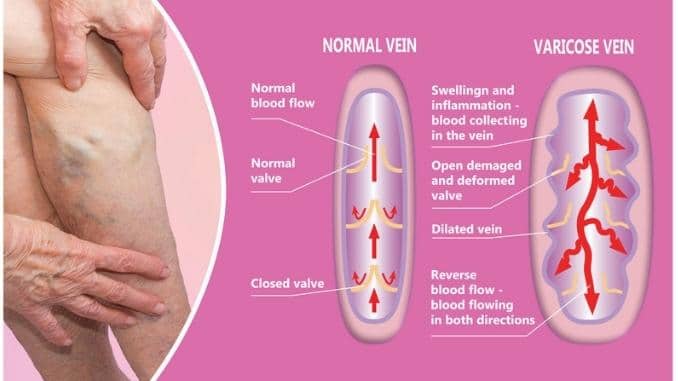
Varicose veins are swollen, twisted veins that lie just under the skin. They’re commonly caused by weak or damaged vein walls and valves.
To better understand what varicose veins are, it helps to know more about how veins work. These are blood vessels that carry deoxygenated blood (blood that no longer contains oxygen) from bodily tissues back to the heart where they can receive a new influx of oxygen.
Veins have to work against gravity to do their job, so they have valves inside them that can open and shut to keep blood from flowing backward. You can think of them as doors that open to allow the blood to go through, then close to ensure it doesn’t drop back down into the ankles and feet.
Over time, as we age and the veins experience wear and tear, they can suffer damage. The vein valves and the vein walls can both become weakened and thin. If blood pressure increases inside these veins—as a result of heart disease—it pushes harder against those damaged areas, causing swelling and distortion.
If the valve fails, blood may flow backward and pool in the vein, causing the veins to stretch or twist. Varicose veins most commonly develop in the legs, because this is where they are most dependent on the valves to keep the blood flowing in the right direction.
What are the Symptoms of Varicose Veins?
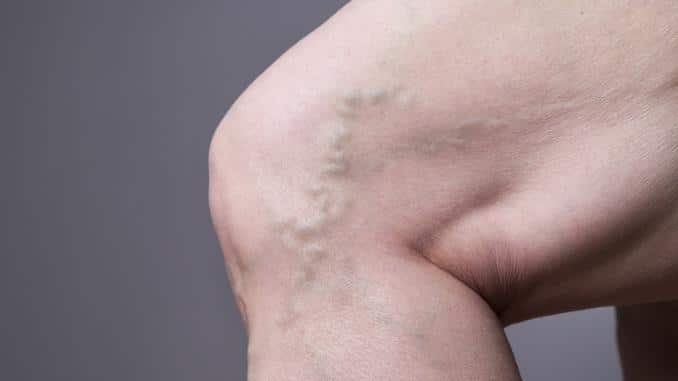
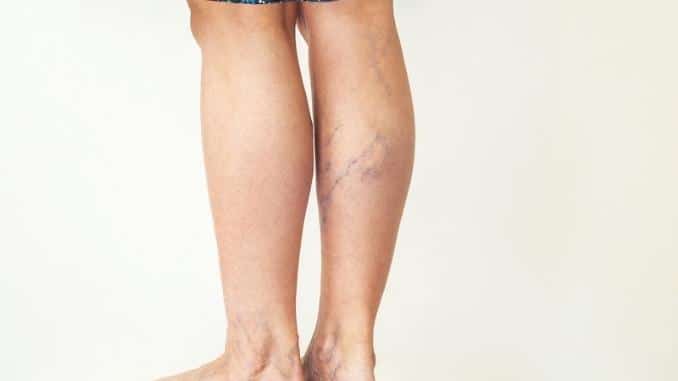
Varicose veins often cause no pain. They do change in appearance, however, becoming dark purple or blue in color, swelling under the skin, and sometimes changing shape into twisted and bulging forms. They may appear like cords on your legs or other areas where they appear, though the legs are the most commonly affected.
Some people, however, feel an aching, heavy sensation in their legs, particularly after walking or standing for a long time. They may also suffer from burning, throbbing, cramping, and swelling in the lower legs, or itching around the veins.
If left untreated, varicose veins can sometimes cause serious complications including:
- Bleeding: Veins near the surface of the skin can bleed, particularly if you bump your leg. This bleeding may be difficult to stop in some cases.
- Blood clots: Since the veins aren’t working as they should, there is a higher risk of blood clots. Should these develop in the legs, they could cause swelling and more rarely, a pulmonary embolism, where the blood clot breaks off and moves to the lungs (a potentially life-threatening situation).
- Ulcers: These are painful sores that can form on the skin near the varicose veins, often near the ankles. These wounds can be hard to heal.
Who Is At Risk for Varicose Veins?
Various factors can increase your risk of developing varicose veins.
1. Family History
Varicose veins do have a strong genetic component. If you have a family history of them, you are more at risk for developing them yourself.
2. Gender
Women are more likely to develop varicose veins than men, though they can affect both genders. Researchers believe that there is a hormone connection, and that hormonal changes during pregnancy or menopause could relax vein walls, causing malfunction.
3. Pregnancy
During pregnancy, hormones change in a woman’s body, and the overall volume of blood also increases. This puts more pressure on the veins to manage all that blood, which can result in extra wear and tear.
Fortunately, pressure is relieved after the birth of the baby and varicose veins may fade on their own. Multiple pregnancies can more greatly increase the risk of lasting varicose veins.
4. Age
The risk of varicose veins increases with age, as the veins start to show some signs of deterioration.
5. Obesity
Being overweight puts added pressure on the veins, making it more difficult for them to pump blood back to the heart while increasing pressure inside the veins. Obesity also increases the risk of other diseases like type 2 diabetes, high blood pressure, and heart disease, all of which contribute to vein damage.
6. Standing or sitting for long periods (desk jobs)
Excessive standing or sitting—particularly when combined with other risk factors—can increase the risk of varicose veins. Both positions, when not changed every 30 minutes or so, can make it more difficult for blood to flow through the veins, causing pooling.
7. History of blood clots
If you’ve had blood clots in the past, or deep vein thrombosis, you are at a higher risk of developing varicose veins. The clots can damage the valves and/or the walls of the veins.
8. Birth control pills or hormone replacement therapy
The estrogen hormone in birth control pills and hormone replacement therapies can weaken the vein valves over time. In the absence of other risk factors, however, this risk is unlikely to cause varicose veins on its own. If you take blood pressure pills and also have high blood pressure, the pills could be an additional risk factor.
Medications and Lifestyle Treatments for Varicose Veins
If you have varicose veins, you’d probably like to get rid of them just so you can feel more confident. But if they’re not causing you any pain or other concerns, your doctor is likely to recommend lifestyle changes rather than medical treatments. These may include the following:
- Elevate your legs: The idea is to give your veins a break so they don’t have to work against gravity so much. Elevate your feet above your heart 3 or 4 times a day for about 15 minutes at a time.
- Wear compression stockings: These elastic stockings assist the veins in getting blood back to your heart. They provide a squeezing effect on the legs, helping to prevent blood from pooling. Wearing these every day can help keep varicose veins from getting worse and may help slightly fade their appearance by reducing swelling.
- Lose weight: Losing some weight can help ease the pressure on your veins. Your doctor may recommend a weight-loss plan or program that can help.
- Stay physically active: Regular physical activity helps keep the blood moving through your veins. Strenuous or vigorous exercise, though, can make them worse, so stick to exercises like walking, biking, swimming, and jogging.
If the lifestyle changes don’t provide enough relief, doctors may prescribe medications. The only drug currently approved for the treatment of varicose veins is diosmiplex—a plant-based medicine that can help ease symptoms like swelling, ulcers, and skin changes. Side effects are typically minor. It can take weeks before you see improvement.

Varicose Veins Treatments and Prevention
People who are experiencing pain from their varicose veins may prefer medical treatments to get rid of them. The options include the following.
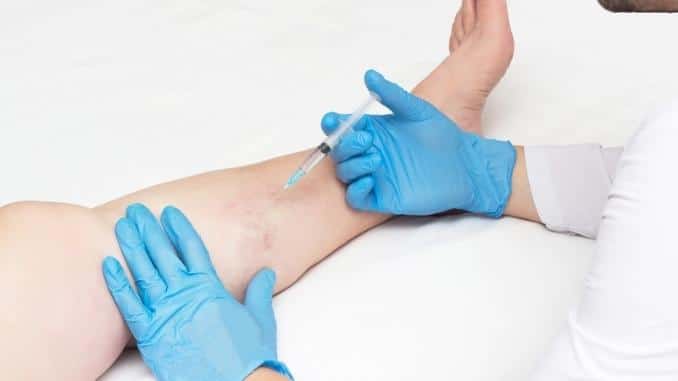
1. Sclerotherapy
This is the most common treatment for varicose veins. It involves injecting a saline or chemical solution into the vein. The solution causes the vein to harden so it no longer fills with blood. Over time, it will die and fade from view. Meanwhile, the body will redirect the blood flow to other veins.
This procedure is most effective for small- to medium-sized veins. It does not require anesthesia and can be done in the doctor’s office. Recovery is typically fast.
For larger veins, doctors may use a variation of this procedure and inject a foam solution of chemicals into the vein to seal it closed.
2. Thermal Ablation
For this procedure, doctors insert a tiny laser fiber into the vein through a catheter and then deliver heat via laser or radiofrequency to destroy the wall of the vein. Afterward, the vein dies and withers away.
Though originally used mostly to treat spider veins in the face, newer laser technology can now effectively treat varicose veins as well.
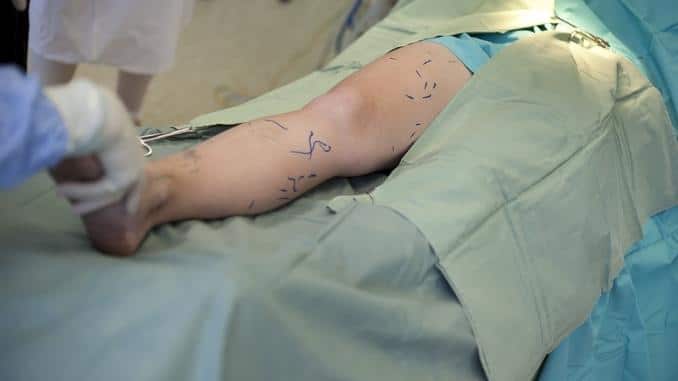
3. Vein Stripping
This procedure is more invasive than the first two, but it can be more effective in treating stubborn varicose veins. The surgeon ties off one vein and then removes it completely through small incisions. The other veins in the leg take over the job of directing blood flow.
This procedure is most often reserved for treating deeper veins in the leg. It may involve more pain and a longer recovery time, so it is usually used only when other treatments fail.
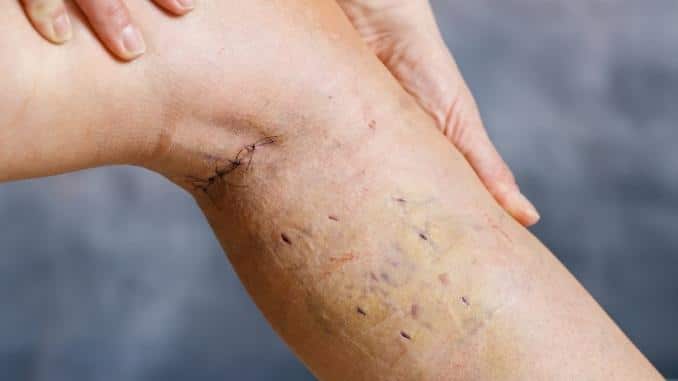
4. Small Incision Avulsion
This procedure is similar to vein stripping but is usually used for smaller veins closer to the skin’s surface. The surgeon makes small incisions, then uses hooks to remove the vein.
5. Transilluminated Powered Phlebectomy
Similar to the procedure above, this one involves the use of suction. A bright light illuminates the vein, and then the doctor employs suction to pull it out. People who have large varicose veins or who are suffering from bleeding or ulcers because of them may be good candidates for this treatment.
Are There Natural Treatments for Varicose Veins?
Some studies have suggested that certain plant extracts may help reduce the leg heaviness and pain that can come with varicose veins. Talk with your doctor first, then consider trying the following:
- Horse chestnut extract—one study found that it relieved leg pain, heaviness, and itching
- Sea pine extract
- Butcher’s broom extract
- Grape seed extract–the National Institutes of Health notes that taking this extract may help reduce swelling in the lower legs
- Sweet clover

Is There a Way to Prevent Varicose Veins?
There’s no way to ensure that you will never have varicose veins. You can, however, adopt some lifestyle habits that can help reduce your risk.
- Exercise for at least 30 minutes a day.
- Maintain a healthy weight; if you’re overweight, try to lose some—even a few pounds can help.
- Eat a high-fiber, low-salt diet.
- Don’t sit or stand in one place for too long—set a timer and get up and walk around and stretch every 30 minutes. If you’re standing, bend and flex your legs to help keep the blood circulating.
- Avoid wearing high heels and hosiery for long periods if possible.
- Try to elevate your legs each day—put your feet up while sitting.
- Avoid wearing tight, restrictive clothing that can impede blood flow.

Remember, although they may be unattractive, in most cases varicose veins do not present any serious medical concerns, so treatment might not be covered under your insurance plan. Do whatever you can to reduce your risks of developing varicose veins and feel free to talk to your doctor about treatment options that are suitable for you as an individual. There are varicose veins treatments and prevention that you can try.
When living a healthy lifestyle you can try varicose veins treatments and prevention from occurring. Click here to learn how to use yoga to stay fit and lower your blood sugar.