Laura figured it was just a rash. Her skin had been dry lately, and she had allergies. She must have touched something she shouldn’t have, or maybe her laundry detergent was bothering her. She shrugged it off, but the next day, it was worse. She checked in the mirror and was surprised to see a wide swath of red skin on her side near her ribs. What had she gotten into?
A few more days passed and the “rash” didn’t get better. It was worse if anything, and now in addition to the redness and irritation, it hurt. Laura didn’t want to wear a bra because the skin was so sensitive, and she couldn’t bear to put on anything but her softest shirts. She wasn’t sleeping well because the pain was waking her up—a stabbing, sharp pain that seemed too intense to be caused by just a rash. By the end of the week, she was feeling miserable and decided she’d better call the doctor.
Laura was surprised when she heard the diagnosis: shingles. Where had that come from? She had taken the Zostavax vaccine a few years before. Unfortunately, though it may have prevented a more severe case, it didn't protect her completely. She asked for treatment, but her doctor told her she was too late for medication to help, as it was effective only when taken within the first few days of the outbreak.
Her doctor did prescribe, however, a special cream to help soothe the rash and the nerves underneath it. Laura went through about a month of discomfort and was relieved when the rash finally disappeared.
According to the U.S. Centers for Disease Control and Prevention (CDC), about one out of every three people in the United States will develop shingles in their lifetime. That’s an estimated one million people who develop it each year. The disease can be painful and, in some cases, long-lasting or even debilitating, so it’s best to protect yourself however you can.
 What Are Shingles?
What Are Shingles?
If you ever suffered from chickenpox, you are at risk for shingles. The same virus causes both diseases. It’s called the varicella-zoster virus (VZV) and is a member of the herpes virus group. Like other herpes viruses, it remains in the body as a latent infection after the first infection. In other words, even after you recover from chickenpox (also called varicella), the VZV remains in your body in a dormant state, just waiting for its opportunity to strike again.
Children and young adults catch the virus through direct contact with someone else who has it, or when a person with the disease coughs or sneezes and the healthy person inhales the air droplets. There is a chickenpox vaccine available that can help reduce the risk of contracting the disease.
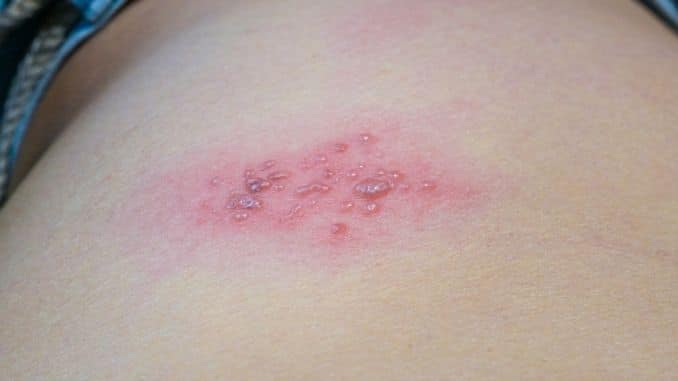
Whether you were vaccinated for chickenpox or not, if you suffered the disease, you are at risk for shingles. The virus remains latent in the nerves and can reactivate later in life and cause a painful rash. In most cases, this rash appears somewhere on the trunk, as it did with Laura, and usually only on one side or another without crossing the middle line. It may also develop on the waistline, face, or side of the head. In some cases, the rash may be more widespread, but this generally occurs only in people with compromised or suppressed immune systems.
The rash may be itchy, tingly, and/or painful. Because the virus lives in the nerves, it causes burning, shooting pain as well as a rash and blisters. The blisters may burst and crust over before they heal. The skin is typically sensitive to the touch, and people may also experience flu-like symptoms, including chills, fever, upset stomach, headache, and body aches.
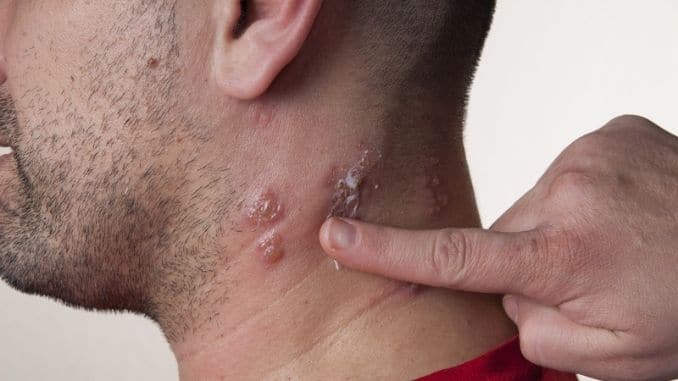 In most cases, symptoms will last for 3-5 weeks, but the severity depends on the person. Whereas some people will experience only mild itchiness and general malaise for a few days, others will struggle with severe pain that comes and goes for several months. Fortunately, most people will have only one episode of shingles during their lifetime, but some can have it more than once or even several times.
In most cases, symptoms will last for 3-5 weeks, but the severity depends on the person. Whereas some people will experience only mild itchiness and general malaise for a few days, others will struggle with severe pain that comes and goes for several months. Fortunately, most people will have only one episode of shingles during their lifetime, but some can have it more than once or even several times.
There is one concerning the long-term effect of shingles called postherpetic neuralgia (PHN). This is a pain that persists in the area where the rash was for more than 90 days. It can last for weeks or months or sometimes, years. The risk of suffering this complication increases with age, as older adults are more likely to have lasting, severe pain. Some medicines can help ease this pain.
Fortunately, extreme complications are rare. The CDC states that only about 1-4 percent of people who get shingles will be hospitalized for it, and about one-third of those suffer more because of weakened or suppressed immune systems. In addition, about 10-13 percent of people 60 years and older who develop shingles will get PHN.
Other rare complications of the disease include:
- Shingles that affects the eye, potentially causing vision loss
- Hearing loss
- Brief paralysis of the face
- Bacterial infection of the blisters
- Nerve damage
- Inflammation in the brain (very rare)
 How Do You Get Shingles?
How Do You Get Shingles?
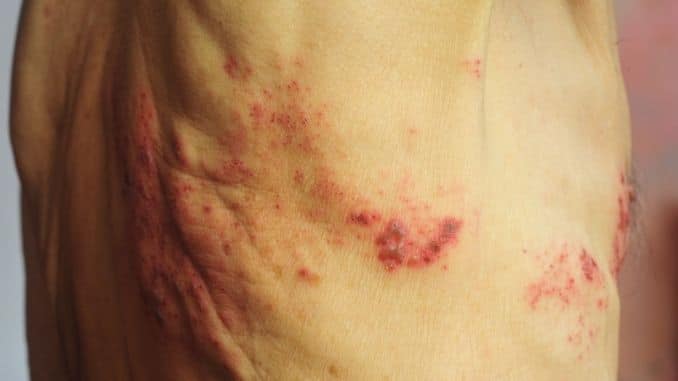
To develop shingles, you must have had chickenpox at some point in your life. That means the virus is inside you waiting for its chance to flourish again. What gives it that chance? One thing: a weakened immune system.
Throughout our lives, the immune system works to protect us from bacteria, viruses, and other invaders that can make us sick. As long as it's strong and working optimally, the virus won't dare challenge it.
But as we get older, the immune system tends to slow down and can also become diminished or weakened, depending on your overall health. That’s why the risk of shingles increases with age—about half of all shingles cases occur in adults age 60 or older. The chance of getting the disease becomes much greater by the age of 70.
In addition to age, other possible causes of a weakened immune system include:
- Cancer
- Human immunodeficiency virus (HIV)
- Bone marrow or organ transplants
- Immunosuppressive medications, such as steroids, chemotherapy, or transplant-related medications
We also know that while both genders are at risk, more women than men develop shingles. We don’t know why. The disease is also less common in blacks than in whites.
 Is Shingles Contagious?
Is Shingles Contagious?
Shingles are contagious but less so than chickenpox, which is more easily transmitted from one person to another.
If you have shingles, direct contact with the fluid from your rash blisters can spread the virus to people who have never had chickenpox or never received the chickenpox vaccine. If they catch the virus from you, they will develop chickenpox, not shingles. The infection that causes shingles is a second-tier infection in all cases. A person who develops chickenpox, however, is also at risk for developing shingles later in life.
To reduce your risk of spreading the virus when your shingles are active, cover the shingles rash with a bandage, and avoid contact with others until the rash heals. It also helps to wash your hands often. Before the rash blisters appear or after they crush over, you are not contagious.
How is Shingles Treated?
If you notice signs of shingles, check with your doctor as soon as you can. There are several antiviral medications that if taken as soon as possible after the rash appears, may be effective in limiting the symptoms and shortening the length of the illness.
Prescription creams, as well, such as the one Laura got, can help ease the stabbing pain associated with shingles rashes. There is no cure for the virus, however, so patients must simply wait it out and allow the body to heal. Over-the-counter pain relievers, oatmeal baths, wet compresses, calamine lotion, and other home remedies can help ease the symptoms.
If you have a rash, your doctor will probably be able to diagnose you pretty easily, but in the absence of a rash, it can be confusing. Shingles often present symptoms similar to other conditions like contact dermatitis, herpes simplex, candida infection, and others. Doctors do have laboratory tests they can use to confirm a case of suspected shingles without a rash.
 The Best Approach: Prevention
The Best Approach: Prevention
There’s nothing good about shingles. It’s painful, aggravating, and sometimes, plain miserable. You want to do all you can to avoid it.
Fortunately, there is a new vaccine for the disease that came onto the market only a few years ago. Before that, the only vaccine we had was Zostavax, which was helpful, but only about 50-60 percent effective in preventing shingles in those 50-70, and even lower for those over 70.
The new vaccine—Shingrix—is 97 percent effective at preventing shingles in people over 50. It also helps prevent PHN and may protect you from the disease for a longer period. Let’s look at some of the other differences between these two vaccines:
| Zostavax | Shingrix |
| Approved in 2006 | Approved in 2017 |
| Live attenuated virus (a weakened version of the virus) | Inactivated vaccine that does not contain live virus |
| Administered into the skin as a single injection | Administered into the muscle in two separate doses with a period of 2-6 months in between |
| Side effects may include irritation and soreness at the injection site | Side effects may include injection site irritation as well as headache, fever, muscle pain, stomach upset, and fatigue |
| Should be avoided in those with compromised immune systems | Can be used in those with weakened immune systems |
| Offers protection for about 5 years, after which effectiveness decreases | Remains effective for at least five years, with studies suggesting it may last longer |
The CDC recommends that people age 50 years and older get the Shingrix vaccine. It can create more side effects than Zostavax, but these typically go away after a day or two, leaving you with a much stronger defense against the disease. Even if you’re not sure whether you had chickenpox when you were younger, scientists still recommend getting the vaccine to protect yourself.
If you've already had shingles, again, the recommendation is that you still go ahead and get the vaccine, as it may help you avoid getting it again. There is no specific length of time you have to wait after having shingles before getting the vaccine, but generally, the recommendation is that you make sure the rash has gone away first.
Those who received Zostavax in the past may also want to get the Shingrix vaccine since it is more effective (and like Laura, even if you had the Zostavax vaccine you could still get shingles). Zostavax is no longer sold in the U.S. as of July 2020.
 Though the vaccine is the only way to truly protect yourself against the disease, you can also increase your defenses by keeping your immune system strong. For more information on how to do that, check out our article, “7 Natural Ways to Boost Your Immune System and Stay Well.”
Though the vaccine is the only way to truly protect yourself against the disease, you can also increase your defenses by keeping your immune system strong. For more information on how to do that, check out our article, “7 Natural Ways to Boost Your Immune System and Stay Well.”
Learn the natural way to boost your immunity. Click here for more information.